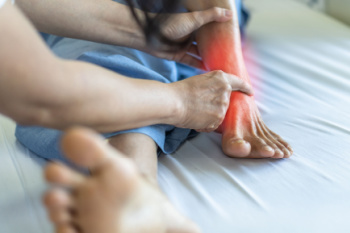
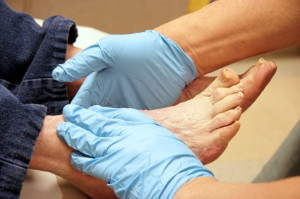
Athlete's foot, or tinea pedis, is a common fungal infection that affects the skin on the feet. It is caused by fungi that thrive in warm, moist environments, such as sweaty shoes or communal showers. Symptoms of athlete’s foot include itching, redness, and a burning sensation, often between the toes or on the soles of the feet. The skin may become dry, flaky, and cracked, which can lead to discomfort and potential secondary bacterial infections. Keeping the feet clean and dry, changing socks regularly, and wearing breathable footwear can aid in recovery and prevent recurrence. For persistent or severe cases, it is suggested you schedule an appointment with a podiatrist for a tailored treatment plan.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact one of our podiatrists from Foot and Ankle Clinics, PA. Our doctors will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our offices located in Woodbury, West St. Paul, and Edina, MN . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.